Investing in Healthy Families
Download PDF of Investing in Healthy Families
A healthy Missouri means all Missouri families can get the health care they need. That sickness or chronic illnesses are caught early, rather than waiting for an emergency to hit. That employees can stay healthy for work, and not spread illnesses unknowingly. That a strong public health network detects problems early, keeping us all safe and well.
A healthy Missouri is a fundamental building block of a prosperous economy and a good quality of life. Yet, Missouri’s investments in critical health care services have significantly declined over the last decade, compromising the health of Missouri families.
Missouri can do better by investing in its greatest resource – its people.
Access to quality health care services allows families to address health care issues on the front end, reducing both catastrophic illness and medical debt. can alleviate chronic diseases, allowing children to be productive in school and adults to be effective in the workforce.
A vibrant public health infrastructure encourages wellness and reduces communicable illness.
A stable and growing health care infrastructure increases access to state-of-the-art care when and where someone needs it, whether in rural or urban areas of the state.
By a variety of measures, Missouri’s health status has declined remarkably over the last two decades. Missourians’ life expectancies are a year and half less than the national average.1 Our children are less likely to have been immunized, and we are much more likely to die of cancer. Not surprisingly, Missouri’s declining health status compared to other states reflects a steep drop in state investments in public health and mental health services:
- An estimated 632,000 Missourians are uninsured; including 90,800 children; yet Missouri’s eligibility limits for medical assistance for low-income Missourians is among the lowest in the nation;
- 1 in 10 Missouri adults have a serious mental illness and 40 percent of those go without treatment; yet, Missouri cut state general revenue funding for mental health services by as much as 35 percent since 2009;
- State funding for local public health agencies has been cut by two-thirds since 2009.
Access to Health Care in Missouri Falls Behind
People with access to health insurance are healthier, live longer and are more productive overall. Those with insurance are much more likely to receive preventive care services including immunizations, annual physicals and prescription medication, all of which can either prevent illness or identify and control chronic illness early leading to better health outcomes.
 One of every nine Missourians, or about 632,000 Missourians are uninsured today. Unfortunately, a combination of cuts to health programs and the decision not to expand Medicaid is making it harder for low-income working families to access health care in Missouri than in most other states.
One of every nine Missourians, or about 632,000 Missourians are uninsured today. Unfortunately, a combination of cuts to health programs and the decision not to expand Medicaid is making it harder for low-income working families to access health care in Missouri than in most other states.
In 2005, Missouri made dramatic cuts to its Medicaid program, causing 100,000 Missourians to lose their health care coverage. The cuts to eligibility remain today. As a result, parents in a family of three that earn more than $301 a month are not eligible for Medicaid in Missouri. At 19 percent of the federal poverty level, Missouri’s eligibility is third lowest in the nation, and well below the national median of 138 percent.
In addition to cutting the number of people eligible for Medicaid, Missouri also cut the services it provides through Medicaid. In particular, dental care for adults has been unfunded for ten years. 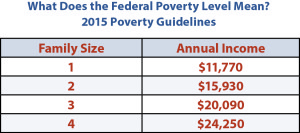
Dental coverage is important not only for oral health, but overall health. Poor oral health is linked to systemic diseases such as coronary heart disease, diabetes, stroke and respiratory disease.3 Lawmakers just recently approved funding for the 2016 state budget year.
Beyond its cuts to Medicaid, Missouri’s inaction on Medicaid expansion has left about 300,000 Missourians without health insurance. While Missouri’s uninsured rate dropped about 25 percent over the last two years, other states have experienced much higher declines in their uninsured rates over the same period.
Missouri Passing By Opportunity to Decrease Uninsured
Nationwide, the decline in the uninsured is largely attributable to the implementation of the federal Affordable Care Act (ACA – otherwise known as “Health Reform”). The ACA included a number of provisions designed to increase access to health care insurance. For example, young adults are now able to remain on their parents’ insurance plans until age 26, and insurance companies are prohibited from discriminating against consumers based on pre-existing conditions.
However, two particular provisions of the law are largely responsible for the dramatic decreases in the uninsured throughout the country since 2013:
Medicaid Expansion: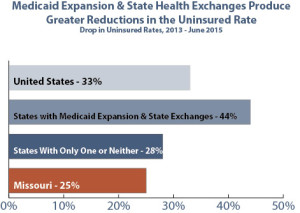
The ACA allowed states to expand eligibility for Medicaid for low-income parents and other nonelderly adults to 138 percent of the federal poverty level.5 No less than 90 percent of the cost of the expanded eligibility group will be funded by the federal government.
Marketplaces:
The law allowed states to set up “Health Insurance Marketplaces,” where people who don’t have access to affordable employer-sponsored insurance can access health insurance plans at reduced costs through subsidies. Citizens in states that did not set up a state-based marketplace have access to a Federal Marketplace.
Recent research by the Gallup organization has found that the number of uninsured Americans dropped 33 percent between 2013 (prior to the implementation of the ACA) and June 2015. But, in states that have chosen to Expand Medicaid and create a state-based Marketplace, the rate of uninsured dropped by 44 percent.6
While the portion of Missourians that are uninsured dropped from 15.2 percent in 2013 to 11.4 percent in June 2015, we can do better. Missouri has not yet taken advantage of the Medicaid Expansion, nor has it created a state-based exchange, resulting in a smaller decline in the number of uninsured compared to other states.
As of July 2015, 31 states and the District of Columbia have adopted the Medicaid Expansion, including several of Missouri’s neighbors: Arkansas, Illinois, Iowa and Kentucky.8 And, seven states, including Iowa, now have uninsured rates below 5 percent.9 However, because Missouri has not yet expanded Medicaid, Missouri’s uninsured rates are more than twice that level.
Very low-income Missourians with incomes below 100 percent of the federal poverty level are not eligible for the subsidies in the exchange. They are also likely not eligible for Missouri’s current Medicaid coverage, which ends at 19 percent of the federal poverty level. In addition, adults in Missouri who do not have children are not eligible for health care assistance through Medicaid no matter how low their income is, unless they are disabled or over 65 years old.
As a result, around 300,000 Missourians now fall into a “health care coverage gap,” in which they cannot access 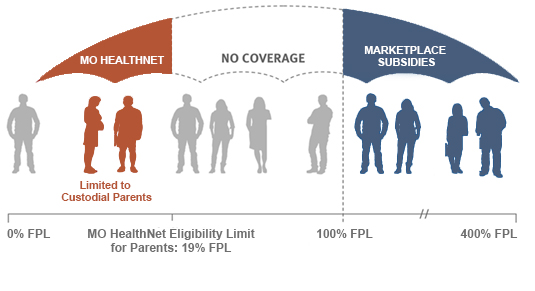 subsidies to purchase health care through an exchange, and they are not eligible for Medicaid. These Missourians include:
subsidies to purchase health care through an exchange, and they are not eligible for Medicaid. These Missourians include:
- 50,000 Missourians with mental illness; and
- 40,000 Missourians with developmental disabilities.10
Further, health providers in Missouri are reporting a cliff in health coverage for children who age-out of Missouri’s Medicaid eligibility. Under Missouri’s current law, teenagers, including those with chronic diseases such as diabetes, lose their Medicaid eligibility on their 19th birthday.11 Because Missouri has not yet expanded Medicaid eligibility, these young Missourians fall into the coverage gap.
Behavioral Health Care Weakening as Public Mental Health Services Critically Cut
One out of every five Missourians suffers from a mental illness.13 But only about half of the people with mental illness have access to and receive treatment for their illness.14 Moreover, one in every 10 adults in Missouri struggles with a serious mental illness each year, which includes diseases such as schizophrenia, bipolar disorder, anxiety disorders and major depression.15
These serious illnesses can often be treated successfully with a combination of medication and psychiatric therapy. However, they are debilitating if left untreated and result in catastrophic community outcomes such as increased unemployment and incarceration rates. In fact, a recent analysis indicates that as many as 385,027 Missourians with serious mental illness go without treatment each year, and untreated mental illness in Missouri results in 46,000 incarcerations, 61,000 unemployed adults, and 274 suicides.16
Missouri’s Department of Mental Health plays a critical role in providing access to mental health care for 170,000 adults and children in Missouri who struggle with mental illness, substance abuse or developmental disabilities such as autism, cerebral palsy, those resulting from head injuries and more. The majority of treatment is provided through a network of 1,800 community-based nonprofit partners that the Department contracts with to provide care.17
 However, state budget reductions made over the last eight years has taken a toll on the ability of these community providers to adequately meet the need for services. Missouri’s spending on public mental health services at $99.40 per capita is well below the national average of $119.62 per capita.18 And, due to Missouri’s low Medicaid eligibility level, only about half of the consumers cared for through the Department’s services are eligible for Medicaid in Missouri. The rest are covered through state general revenue-funded programs, which have faced the most significant reductions made to mental health funding in the state budget.
However, state budget reductions made over the last eight years has taken a toll on the ability of these community providers to adequately meet the need for services. Missouri’s spending on public mental health services at $99.40 per capita is well below the national average of $119.62 per capita.18 And, due to Missouri’s low Medicaid eligibility level, only about half of the consumers cared for through the Department’s services are eligible for Medicaid in Missouri. The rest are covered through state general revenue-funded programs, which have faced the most significant reductions made to mental health funding in the state budget.
Since 2009, state general revenue funding for non-Medicaid community mental health services for uninsured adults has been cut by 35 percent.
The combination of budget reductions to community services for adults with mental illness and flat funding in other mental health services is stretching providers. In fact, over the last decade, the reimbursement rates for the Department of Mental Health’s community providers have fallen far behind inflation, making it harder for providers to maintain proper staffing and services:
- Reimbursement rates for providers of community mental health services have fallen 27 percent below inflation;
- Rates for providers of services for developmental disabilities have fallen 24 percent below inflation; and
- Reimbursement rates for providers of substance abuse services have fallen 25 percent below inflation.19
Moreover, the state budget reductions are compromising access to care. Patients are experiencing increasing wait times to access psychiatric care, and waiting lists for some services have developed. For example, as many as 302 patients are currently on a waiting list to access in-home services or residential care for developmental disabilities through the Department of Mental Health.20
There are serious consequences to Missouri’s reductions in public mental health funding. If left untreated, serious mental illness can escalate and result in premature death, increased incarcerations, create burdens to county jails and law enforcement agencies, and increased costs for Missouri taxpayers:
“In Jefferson County we are seeing a lot more mentally ill people and substance abusers in our county jail who would be better dealt with by a mental health center. Our local mental health center does not have the capacity to take care of all those who need care in a timely basis. Forensic evaluations are very difficult to get and when we need to take someone to a hospital for a 96 hour hold it removes a deputy from other duties and therefore affects public safety.”- Sheriff Glen Boyer of Jefferson County21
Early intervention services for mental health and substance abuse treatment can instead reduce the costly consequences of untreated mental illness. For instance, the average prison stay for a drug offender in Missouri costs $19,041. The average cost of community-based mental health treatment is only $1,771.22
Missouri’s Public Health Investments Suffer
 During the peak of the Ebola outbreak, the online magazine Slate posited that Missouri is the worst place in the country to get Ebola.23 Why? Because its public health investments rank 50th in the nation. And the public health infrastructure is what we rely on to monitor and detect disease outbreaks.
During the peak of the Ebola outbreak, the online magazine Slate posited that Missouri is the worst place in the country to get Ebola.23 Why? Because its public health investments rank 50th in the nation. And the public health infrastructure is what we rely on to monitor and detect disease outbreaks.
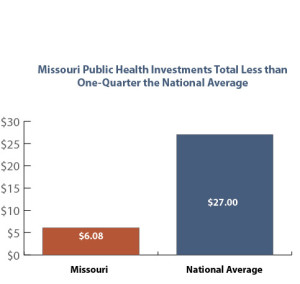
While its headline was attention-grabbing, it underscores an important fact: Missouri spends less than one-fourth the amount that most other states spend on public health services.25 Missouri spends just $6.08 per person in state funding for public health, while the national median amount is $27.40.
Missouri’s network of 115 local public health agencies address a wide range of public health issues, including evaluating environmental health risks, providing emergency services during natural disasters, controlling for communicable diseases such as the flu, overseeing food safety and providing public education to enhance the health of the community.26 Although public health funding represents less than two percent of all health care spending, its impact is extensive, resulting in decreased rates of tobacco use, improvements in nutrition and physical activity.27
 Unfortunately, Missouri’s investment in public health services has dwindled over the last decade, resulting in significant cuts to funding for local public health agencies.
Unfortunately, Missouri’s investment in public health services has dwindled over the last decade, resulting in significant cuts to funding for local public health agencies.
More than half of the local public health agencies have been forced to cut programs, health educators have been lost in many counties reducing the community education programs that the agencies can provide in local communities on healthy behaviors and smoking cessation and classes which help people manage their chronic health conditions such as diabetes or arthritis.28
Moreover, Missouri’s rank in health outcomes has declined considerably over the last two decades. In 1990, Missouri  was ranked as the 24th healthiest state, but by 2014 Missouri dropped to 36th in the nation.29 The United Health Foundation measures a variety of factors which collectively determine the level of health within a state. The indicators include behavioral factors such as smoking rates, environmental factors such as the prevalence of infectious disease, policy factors including public health funding and immunization requirements, access to clinical care including primary care physicians and dentists, and outcomes including premature deaths.
was ranked as the 24th healthiest state, but by 2014 Missouri dropped to 36th in the nation.29 The United Health Foundation measures a variety of factors which collectively determine the level of health within a state. The indicators include behavioral factors such as smoking rates, environmental factors such as the prevalence of infectious disease, policy factors including public health funding and immunization requirements, access to clinical care including primary care physicians and dentists, and outcomes including premature deaths.
Moving Forward
A healthy Missouri is a fundamental building block of a prosperous economy and a good quality of life. Yet, Missouri’s investments in critical health care services have significantly declined over the last decade, compromising the health of Missouri families. Missouri can do better by investing in its greatest resource – its people.


