MO HealthNet – Missouri’s Medicaid program – is funded jointly by the federal and state governments. The amount of the federal share, or the FMAP (Federal Medical Assistance Percentage), is currently 65% in Missouri. The federal government has temporarily increased its match for the traditional Medicaid program to respond to the public health emergency (PHE) and to incentivize Medicaid expansion. The chart below illustrates the how these temporary enhanced match rates apply to MO HealthNet, and how the timing differs from the permanent match rate that applies to the Adult Expansion Group.
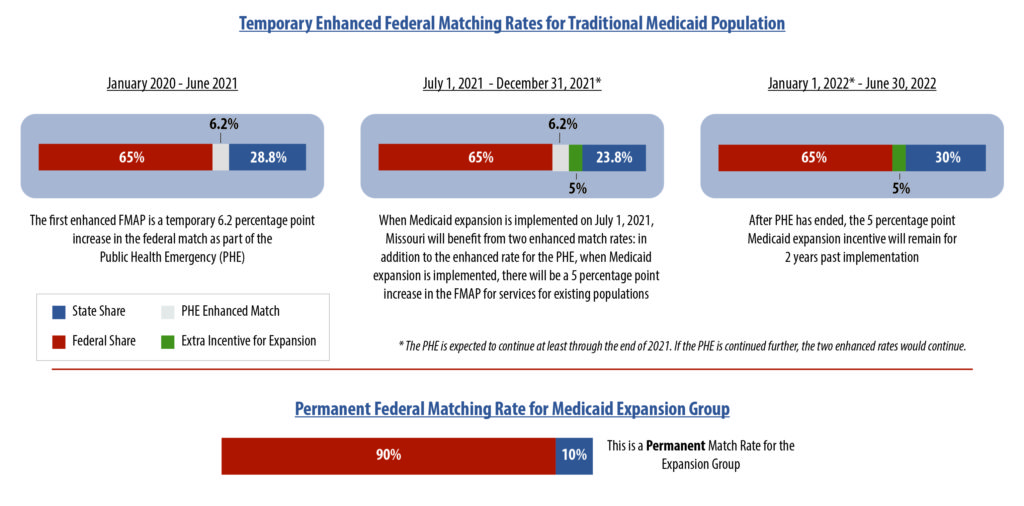
Temporary Increases to the Federal Match Rate
While it may vary slightly from year to year, Missouri is generally responsible for around 35% of the costs for the current Medicaid program, while the federal government pays for about 65%. (Note: Provider taxes cover a significant portion of the state share, with GR funding less than 20% of total Medicaid costs).
Enhanced FMAP Tied to the Public Health Emergency
- The Families First Coronavirus Response Act, (March 2020) temporarily increased the federal match rate by 6.2 percentage points. This match rate applied beginning January 1, 2020 and will continue until the end of the PHE.
- In a letter to states, the Biden Administration indicated that it expected the PHE to continue at least through the end of the calendar year.
- This enhanced match is expected to deliver an additional $376 million to Missouri in state fiscal year 2022.
Increased Federal Match for Traditional Medicaid (Tied to Expansion Implementation)
- The American Rescue Plan Act (March 11, 2021) provides states that have not yet expanded Medicaid a 5 percentage point increase in the Federal Medical Assistance Percentage (FMAP) for its existing Medicaid program, for a period of two years after expansion is implemented.
- Although Missouri voters have already approved Medicaid expansion, because it has not yet been implemented, Missouri will benefit from this enhanced FMAP beginning when expansion is implemented on July 1, 2021 (through June 30th, 2023).
- Missouri’s estimated funding for this enhanced Medicaid match is $1.15 billion.
Both of these match rates will apply to services for MO HealthNet’s already existing population groups for the period of time after expansion until the Public Health Emergency ends.
Permanent Match for Medicaid Expansion Population
- Medicaid expansion will provide access to health care to Missourians earning less than 138% of the federal poverty level (about $18,000 for an individual, or $30,000 for a family of three).
- The federal government will fund 90% of the cost of this group.
- While the federal government has often increased its contribution to Medicaid during economic crises, it has never reduced the formula for its permanent rate.
A previous version of this report was published prior to the passage of the American Rescue Plan Act, which provided an additional enhanced federal match as an incentive for Medicaid expansion. The earlier version is available here.

